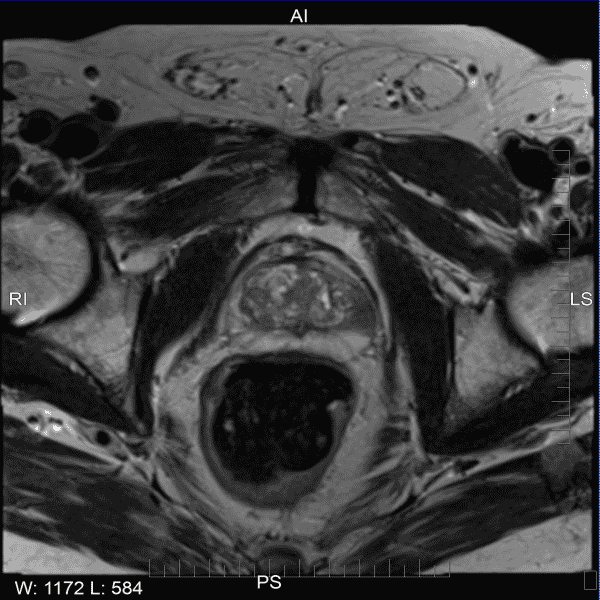
MRI Prostate Cancer Part2
Norby
Norby
Results of my MRI explained.
Exam Description:
MRI Prostate with and without IV Contrast
1. MRI with and without IV Contrast
Excerpt:
Over the past few years, multiparametric MRI (mpMRI) of the prostate has emerged as the most successful radiologic imaging study for detecting prostate cancer. The PI-RADS system and the MRI pathway have paved the way for a widespread usage of this imaging test in daily clinical practice [1]. Prostate MRI is on the verge of opening up further indications towards screening, which is quite remarkable. As a result, the number of prostate MR scans has increased sharply and this trend will continue in the next years. This puts pressure on the justification to perform the most invasive and “controversial” part of MRI of the prostate, the dynamic contrast-medium-enhanced sequence.
2. Gadolinium-based contrast agents (GBCAs)
Excerpt:
Gadolinium contrast agents- challenges and opportunities of a multidisciplinary approach: Literature review.
Contrast agents is used in magnetic resonance imaging (MRI) to improve the visibility of the details of the organ structures. Gadolinium-based contrast agent (GBCA) has been used since 1988 in MRI for diagnostic and follow-up of patients, the gadolinium good properties make it an effective choice for enhance the signal in MRI by increase its intensity and shortening the relaxation time of the proton.
Clinical history:
Biopsy-proven prostate cancer, Gleason score 3+4=7, on active surveillance.
Most resent PSA: 5.86 ng/mL on 02/16/2026.
If available, previous MRI information is compared with the current MRI to see the current changes. In my case we have the Gleason score and the latest PSA number.
Technique: This is a layout test from Norby
Multisequence multiplanar MR imaging of the prostate gland was performed on a 3 Tesla magnet. Precontrast 3-plane high-resolution T2-weighted images, axial T1-weighted images, and axial diffusion weighted images with ADC maps of the prostate were obtained. Axial T1, T2, and fat-suppressed T2-weighted images of the whole pelvis were obtained. Dynamic post contrast imaging of the prostrate gland was performed following administration of 12ml Dotarem intravenously. Post processing and gland segmentation was performed on a DynaCAD workstation.
1. Multisequence multiplanar MR imaging
Excerpt:
Multiparametric-magnetic resonance imaging (mp-MRI) has shown promising results in diagnosis, localization, risk stratification and staging of clinically significant prostate cancer. It has also opened up opportunities for focal treatment of prostate cancer. Combinations of T2-weighted imaging, diffusion imaging, perfusion (dynamic contrast-enhanced imaging) and spectroscopic imaging have been used in mp-MRI assessment of prostate cancer, but T2 morphologic assessment and functional assessment by diffusion imaging remains the mainstay for prostate cancer diagnosis on mp-MRI. Because assessment on mp-MRI can be subjective, use of the newly developed standardized reporting Prostate Imaging and Reporting Archiving Data System scoring system and education of specialist radiologists are essential for accurate interpretation.
Precontrast 3-plane high-resolution T2-weighted images
Excerpt:
of scan is best used for.
Axial T1, T2, and fat-suppressed T2-weighted images of the whole pelvis were obtained
Excerpt:
of scan is best used for.
Findings:
Prostate:
Measurement: 5.2×3.7×4.8cm. Estimated volume: 47.4 cc, previously 37.2 cc. PSA density 0.12 ng/ml/cc, previously Prostatic density: 0.24 ng/mL2.
Quality: Motion degrades image quality and limits evaluation.
Postbiopsy hemorrhage: None.
Peripheral zone: Multifocal linear and wedge-shaped T2 attenuation of the peripheral zone likely related to scarring and/or sequela of prostatitis.
Transition zone: Multiple heterogeneous nodules consistent with prostatic hyperplasia.
5. Estimated volume: 47.4 cc, previously 37.2 cc
Excerpt:
What is a Normal Prostate Volume?
In healthy adult males, the normal prostate gland measurement is approximately:
Width: 1.6 inches (4 cm)
Height: 1.2 inches (3 cm)
Depth (thickness): 1 inch (2.5 cm)
This results in a prostate that weighs about 0.7 to 1 ounce or 20 to 30 grams. The total prostate volume is 20 to 30 cubic centimeters (cc). For comparison, that’s about the size of a walnut.
Its size allows the prostate to carry out its primary function, which is to produce seminal fluid that nourishes sperm and supports ejaculation.
5. What can be done to reduce volume?
I am looking for an answer. A 27% increase in volume is not good. the question is: What can be done to reduce the size and or to slow down the growth naturally?
I am still looking for results.
Norby
6. PSA density change from 0.24 to 0.12 ng/ml/cc
Excerpt:
Understanding PSA Density and Prostate Cancer
What is PSA Density?
Prostate-specific antigen (PSA) density is calculated by dividing the PSA level by the prostate volume. This metric helps assess the risk of prostate cancer more accurately than PSA levels alone. A higher PSA density indicates a greater likelihood of prostate cancer, while a lower density suggests a lower risk.
Impact of Lower PSA Density
Prognosis: Men with lower PSA density generally have better survival rates. This is because lower density often correlates with less aggressive forms of prostate cancer.
Treatment Decisions: Patients with lower PSA density may require less aggressive treatment options. This can include active surveillance rather than immediate intervention.
MRI evaluations
Focal Lesions:
Lesions #1:
Locations: Left, anterior peripheral zone midgland to base.
Size: 10 mm (series 4 image 17), previously 5 mm.
T2: Score 4. Heterogeneous moderate hypointensity.
DWI/ADC: Score 3. Moderately hyperintense on DWI and markedly hypointense on ADC.
Mean ADC value -0.655 x 10-3 mm2/s.
DCE: Positive.
Extraprostatic extension: Equivocal. Board capsular contact is present.
PI-RADS score: 4. PIRADS 4 High (clinically significant cancer is likely to be present).
Neurovascular bundle: Unremarkable
Seminal vesicles: Unremarkable.
Urinary bladder: Urinary bladder wall thickening, likely sequela of chronic outlet obstruction.
Rectum/Colon: There is colonic diverticulosis and increased stool in the colon.
Lymph nodes: No pathologically enlarged lymph nodes.
Bones: No aggressive osseous lesions.
Other: No significant pelvic free fluid. Small fat-containing left inguinal hernia.